In a recent Axway consumer survey, we found many Americans are taking advantage of growing interoperability in healthcare, but there’s still work to do to put patients in control of their health data. The survey asked 1,017 American adults from a representative sample about their general understanding and concerns related to their digital healthcare experiences and how they feel healthcare partners serve them and protect their data. Read on for an overview of the results.
Healthcare interoperability deadlines are upon us
Interoperability mandates mean healthcare now needs to be open for business with APIs. But merely complying with government regulation would be missing the mark: we have such an opportunity to build better experiences, much faster.
Healthcare interoperability is at an inflection point in the United States, where the Department of Health and Human Services now requires healthcare partners to liberate patient data to drive patient access to health information.
Healthcare partners must adopt HL7 FHIR APIs to open up patient data, first and foremost to patients themselves, and also to allow for sharing data with third parties, such as healthcare app developers. The CMS Interoperability and Patient Access Final Rule includes information blocking provisions so patients remain in control of their data.
Other requirements are fast approaching, all of which build on the technologies required by previous rules. CMS will begin enforcing certain provisions of the Transparency in Coverage Final Rules in mid-2022, with the rest rolling out incrementally through 2024. The No Surprises Act, which establishes new federal protections against surprise medical bills, takes effect in 2022, and price comparison tools should start making their appearance in 2023.
Patients want access to their data, and healthcare is missing opportunities
In our survey, we found Americans want what APIs in healthcare can offer: better access to and ownership of their health records. And they also have some reservations about privacy.
The good news is nearly half of the respondents (46%) feel their healthcare portals and websites were easy to use, and 64% feel they usually give them access to the information they were looking for. And most people (66%) are happy to fill out medical forms online or in a mobile app to avoid filling out more paperwork.
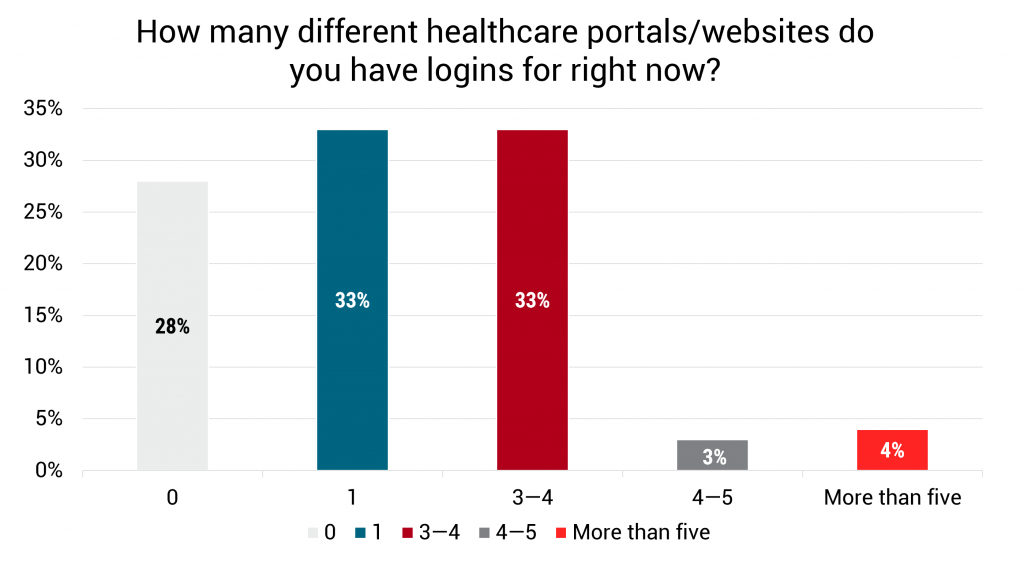
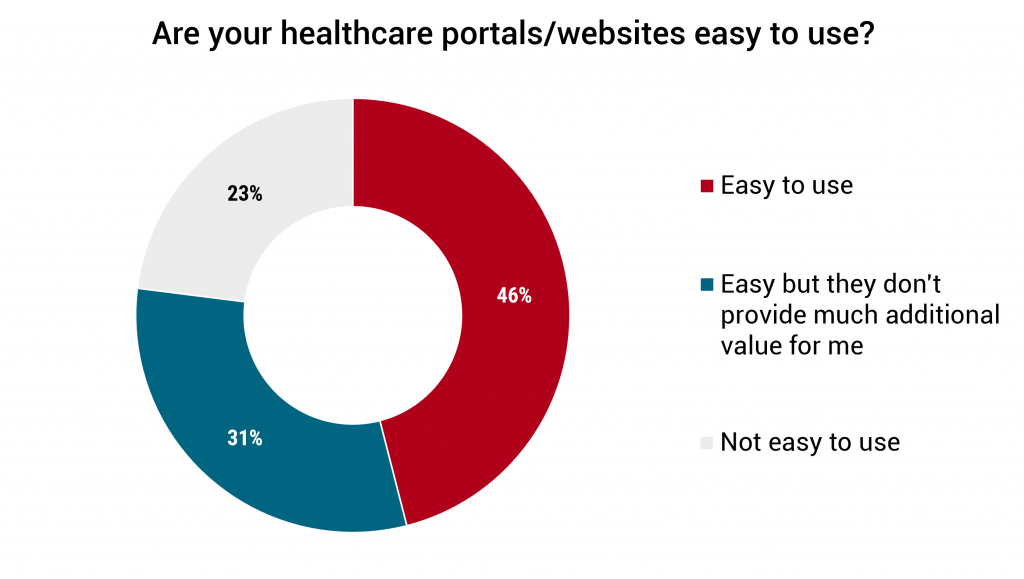
But the survey also highlights missed opportunities for better customer experiences: 31% of respondents said these portals — while easy to use — didn’t really provide any additional value to them. 36% said they don’t provide the information they’re looking for, and for nearly 25% of respondents, it was hard to navigate their online healthcare portals.
Healthcare portals aren’t delivering on their promise: the GAO reports that nearly 90 percent of providers are offering access to a patient portal, but less than one-third of patients have used theirs. In large part, there simply wasn’t enough buy-in from healthcare partners.
The interoperability rule could drive expanded use of these portals, making them more customer-friendly and more useful too. Portals could open doors to digital conversations between clinicians and patients, for example: going beyond the telehealth visit, patients could ask their doctor questions about medications and allergies.
We have such an opportunity to truly transform the patient experience and offer better value with these digital experiences. Instead of half-heartedly adopting FHIR solely to check a regulatory compliance box, we can see this as a chance to lay a foundation and build all sorts of new things on top of it that we’ve never been able to do before.
The developer experience needs to change
What is really changing for health providers and health payers is that they must transform how they think of integration. In the past, every integration was a project-based integration.
Now, we’re moving from costly, project-based integration to open APIs, in real time. And that means partners have to completely rethink the developer experience and move toward treating their APIs as a self-service platform for developers.
Developers need to be able to get their security tokens and get their applications registered, then programmatically, without having to ask anyone, download and test them — and finally move to production via an API portal.
Right now, in healthcare, everything is still very project-based. People get on a phone call, they talk through it, and there’s a project manager from both sides. It’s very much the same way we’ve done integrations for 20 years.
The interoperability rule means that healthcare has to act like a marketplace for developers. Healthcare providers and payers and partners need to be participating in an ecosystem.
All this means healthcare administrators need to learn to let go of control to some degree, which is a big shift. They are understandably used to being very careful about security and privacy reasons, but opening up healthcare means they have to rely on secure solutions. They need proven API Management systems that can secure APIs and manage traffic.
Patients now have the right to download all of their health data to an application of their choice – these payloads can be quite large and occur at unexpected times. Healthcare administrators need a strong proven platform to manage API traffic.
Security remains top of mind
Building on a secure foundation means healthcare organizations and patients don’t need to worry about data breaches and data leakage. An API-first approach gives your healthcare organization the tools to create, manage, and scale your APIs and securely open channels to the healthcare ecosystem, including third-party developers.
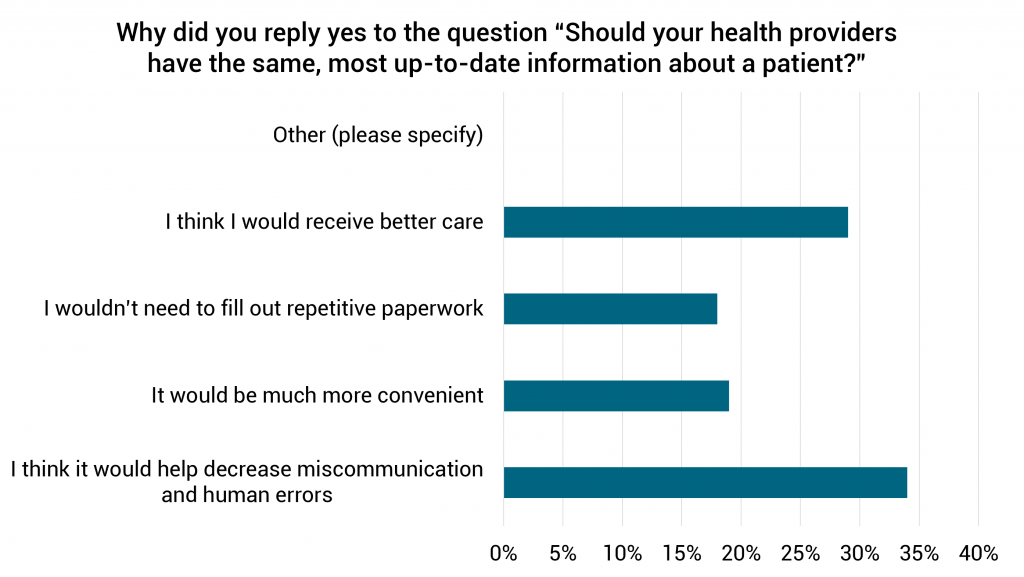
Our survey found nearly three-quarters (74%) of Americans agree their health providers should have the same, most up-to-date information about a patient to help decrease miscommunication and human errors and provide better care.
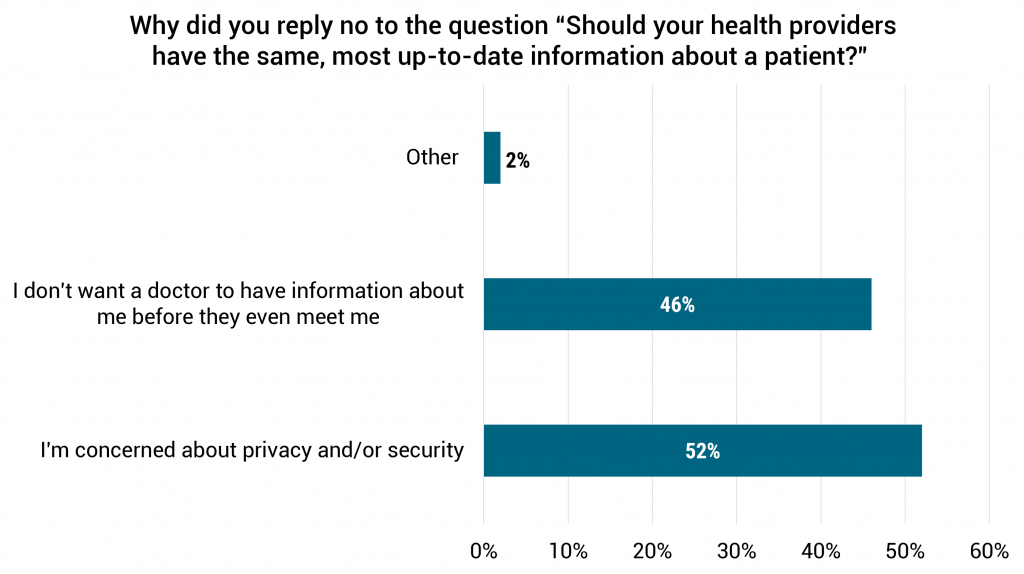
But the 26% that disagree are worried about their privacy: half of these worries about doctors having access to information about them without even meeting them, and the other half worry about their security and privacy.
The interoperability rule is designed to protect patients because it puts the data in their hands and gives them control over who they want to share it with.
To build that trust, healthcare partners need to put in the energy up front to improve their customers’ experiences, help people understand it through education, and train all the teams involved in the people-process along the way.
We’re only beginning to scratch the surface of innovation in healthcare
Taking the interoperability rule as an opportunity to innovate and speed up processes can result in truly transformative solutions. More changes are coming with interoperability regulations in the U.S., and with that, more opportunities to transform the patient experience.
Imagine, for example, being able to speed up prior authorization.
As things are now, typically with electronic prior authorization, we still have to go to a portal and send our documents manually. We still have to go through a couple of days, if not weeks, cycling through submitting forms, waiting for an assessment, checking on the status, getting an update, maybe making another change, submitting the forms again…
Sometimes, time is of the essence — if you’re suffering from what may be aggressive cancer, you don’t want to be waiting for weeks to get more lab work approved.
With a prior authorization API, we could move faster because we could also share all the data to support that decision electronically. That’s a game-changer for the patient, who could receive timely, life-saving treatments faster.
API-first is the key to real transformation
The CMS interoperability rule could help drive transformative solutions. But true interoperability will require adopting API-first and design thinking to better serve patients and partners.
We are seeing a steady progression to opening up our data repositories and securely sharing that information. We should use this foundation to innovate — delivering new services to improve health outcomes and to help patients take control of their healthcare experience.
Click here to read the full survey results.
Learn more about opening up for innovation in healthcare with the eBook, “Turning interoperability into opportunity.”

Follow us on social